CHR and Community Health Workers Building a “Bridge to Health” for Underserved Diabetes Patients
Stories - Feb 14 2019

Diabetes can take a tremendous toll on the lives of the patients it affects, especially those from underserved communities or those with limited access to services. According to the Centers for Disease Control and prevention, approximately 40% of American adults are living with diabetes or prediabetes, and many with diabetes aren’t properly managing their chronic disease. Now, work at Kaiser Permanente’s Center for Health Research (CHR) aims to assess interventions that might help patients in need better manage their type 2 diabetes. Thanks to a two-year federal grant from the National Institute for Diabetes and Digestive and Kidney Diseases (NIDDK), CHR will assess the impact of addressing social and economic needs and providing disease self-management training on both low-income patients and those from racial or ethnic minority backgrounds with poorly managed diabetes.
 Dr. Fitzpatrick’s research centers on facilitating behavioral change among people with obesity and those with diabetes and cardiovascular disease.
Dr. Fitzpatrick’s research centers on facilitating behavioral change among people with obesity and those with diabetes and cardiovascular disease.
Stephanie L. Fitzpatrick, PhD (right), the researcher at CHR leading the study (called Bridge to Health or Puente a la Salud in Spanish), involves not only Kaiser Permanente patient navigators, but community health workers as well, in the effort to reach patients and test two pragmatic interventions to identify the best way to improve their health outcomes. The project looks at whether it’s more beneficial to patients’ health to address their social and economic needs and provide intensive training in diabetes self-management skills or whether it’s enough to address their social and economic needs alone, using a reduction in A1C as the measure. A test for A1C is the primary measure used by health care providers in diabetes diagnosis and management. The study team will recruit 100 participants for the study, which—because it will be tested under real-world conditions—has a high potential for implementation.
In addition to the KP navigators, the community health workers involved in the project come from eight Portland, Oregon-area nonprofits —Latino Network, Familias en Acción, Volunteers of America Portland, Northwest Family Services, Impact NW, Portland Opportunities Industrialization Center, and Immigrant and Refugee Community Organization, and El Programa Hispano Catolico. Project Access NOW, a major community partner for the Bridge to Health Study, will help facilitate referrals to the community health workers at these agencies.
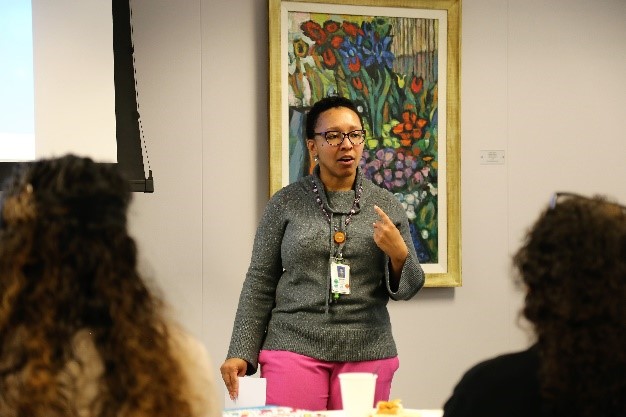 Dr. Fitzpatrick (above) leading the training of community health workers in January.
Dr. Fitzpatrick (above) leading the training of community health workers in January.
The health workers from these organizations joined the team from KP and participated in four days of training in January, which ranged from learning more in-depth information about diabetes management to strategies for counseling participants on health behavior change. In addition, they received training in a curriculum developed at Johns Hopkins by Felicia Hill-Briggs, PhD, ABPP, called DECIDE (Decision-making Education for Choices in Diabetes Everyday), a self-paced program that helps people with diabetes learn problem-solving skills and change diabetes-related behaviors. Dr. Fitzpatrick was taught DECIDE during her postdoctoral fellowship at Johns Hopkins with Dr. Hill-Briggs and was an interventionist for the NIH-funded clinical trial that studied the effect of implementing DECIDE among the urban African American population with type 2 diabetes.
The organizations involved and KPNW all have something to gain from this partnership: KPNW is benefiting from the workers’ deep knowledge of the communities and individuals they work with, while the health workers are adding new knowledge and skills to their care “toolbox” to help these patients. One of community health workers who participated in the training, Pilar Lashley of Familias en Acción, even said that she called two of her clients the evening after the first training because of insights she’d gained in a role-playing exercise.
Dr. Fitzpatrick’s research centers on facilitating behavioral change among people with obesity and those with diabetes and cardiovascular disease.
Dr. Fitzpatrick wrote the grant after getting involved in the evaluation efforts of the Regional Community Health Network – comprising Kaiser Permanente Northwest, Providence Health & Services, and Oregon Health & Science University – which has a goal to better align health systems and community-based agencies to increase the connection of patients with diabetes to community resources. She acknowledges KP Community Health for spearheading Kaiser’s involvement in this Network and inviting her to be a part of this important initiative.
“Social determinants of health such as food insecurity, inadequate housing, and financial stress are major barriers to optimal diabetes management and contribute to health disparities,” explained Dr. Fitzpatrick. “The goal of Bridge to Health is to see if we can address the social and behavioral barriers while reducing the disparities gap among our most vulnerable members by extending diabetes care outside of clinic walls and into the community with the use of community health workers.”